Company Name
Confidential
Industry
Funeral Home
Location
New Jersey
Employee Headcount
46
Small Group Medical Plans
A group medical plan is considered to be underwritten in the small group marketplace if the number of enrolling lives is less than 50 or 100, depending on the state you operate in. For most companies, your plan will be underwritten out of the state where the company is headquartered or where a majority of enrolling employees work. The state in which you create a group medical strategy will dictate what strategies are available to your company, and more importantly, how the pricing will work itself out. If you have less than the mandated lives to qualify as a large group, you will be underwritten in either a state that provides age-based rates or composite (also known as community) rates. Without proper guidance, determining the right approach is very challenging for a benefits administrator.
New Rates, Same Problem
A company based in New Jersey with 46 employees was originally advised to choose a fully-insured health plan for their employees. While this type of plan worked well for the group while they were a boutique sized firm, they started to grow out significantly. One of the primary challenges of being a small employer in New Jersey and creating a medical plan is the way that traditional insurance companies price their plans. Exhibit 1
As with prior years, the insurance programs renewal rates reflected an increase. According to the Kaiser foundation, the average increase for employer-sponsored health insurance costs in 2019 were 4%-5% for individuals and families respectively. In this clients case, the renewal rates increased by 7-9%. This rate represented a significant increase and pushed the employer costs well out of their projected fiscal budget.
Due to the nature of this strategy, no transparency is provided regarding claims experience and it is difficult for a group to determine if the cost increase is due to their losses or the overall market they operate in. It was at this point that the client had engaged our firm to review their options and evaluate alternative solutions.
Premiums with Potential
In the due diligence process, we were able to determine that the coverage was sufficient, but it was the pricing and lack of transparency that left the client frustrated. It became a challenge when considering new employees as each employee would be paying a slightly different premium for their plan.
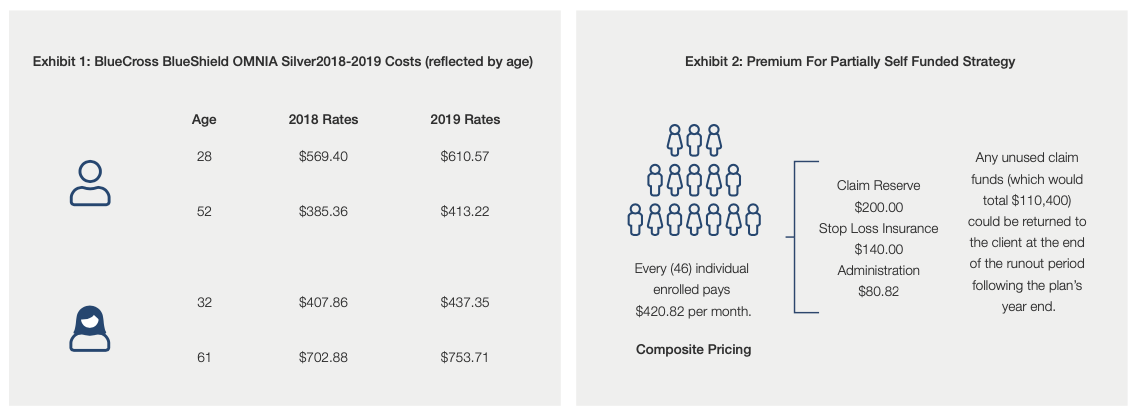
It was at this point that Bona Vita Benefits introduced partially self funded medical plans with stop loss insurance. This type of program is priced based on the demographics and health of the overall group. By being underwritten in this fashion, the insurance program can provide composite pricing which will streamline both an employer funding strategy and administration of the plan.
In addition to the benefit of creating a composite based pricing model, there is the potential for a return of unused accumulated claim funds. The premium Exhibit 2 paid in this type of strategy is divided into three categories; claim reserve funding, stop loss insurance premium, and administration.
Claim Reserve Funding
A portion of the premium will be allocated toward a reserve fund which will produce the funds to pay for claims experienced by the group. If an employee sees a doctor and pays $35 for the visit, this claim fund will reimburse the provider for the services rendered up to the negotiated rate. At the end of the year, there is generally a run-out period. This requires a group to wait for up to six months for the return of claim funds. A group may elect to receive 50% or 100% of any unused funds that remain.
Stop Loss Insurance Premium
The program provides protection in the event catastrophic losses arise and the claims that come in go above and beyond the accruing claim fund. This insurance can be provided on an aggregate level which means it applies to the total claim reserve fund. It can also apply on an individual level to any single employees claim experience. This type of coverage is known as Individual Stop Loss Insurance.
Administration
This is the cost associated with building the plan, administering the plan throughout the year, paying claims experienced and the cost of any brokerage commissions.
Bottom Line
Bona Vita Benefits was able to provide the client savings, as well as a strategy with a simplified pricing and potential for a return of unused claim funds.
This is a hypothetical situation based on real life examples. Names and circumstances have been changed. The opinions voiced in this material are for general information only and are not intended to provide specific advice or recommendations for any individual. To determine which investments or strategies may be appropriate for you, consult your advisor prior to investing.
